Whiplash associated disorder or WAD is a familiar and common result of a car accident and a cause of significant costs in lost work, disability, pain and medical care. It is the result of a stretch injury to the ligaments and muscles of the neck. Other causes can be falls, horse riding accidents, sports injuries or assaults.
Neck pain is common with 70% of adults reporting an episode at some time in their lives. It appears to be increasing in frequency and increasing in costs as social, work and travel changes impact upon our welfare.
Scientific work has shown that whiplash is a complex condition that varies considerably in its physical and psychological characteristics and which has widely varying treatment outcomes.
It is important to realise whiplash sufferers are different from people with standard neck pain and need managing accordingly.
Whiplash Symptoms
Many different symptoms are described after a whiplash injury and may be present at the time or be delayed for twelve hours or more:
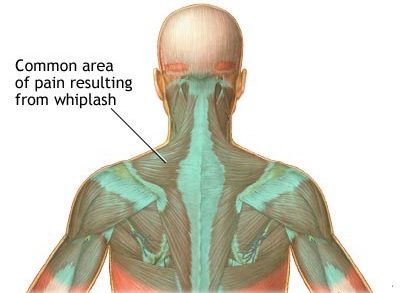
- Neck pain at the back of the neck. Pain can also be in the head, shoulder, arm, shoulder blade, thoracic and low back areas.
- Headaches and dizziness
- Poor balance
- Visual disturbance
- Muscle weakness
- Abnormal feelings such as pins and needles and numbness
- Memory and concentration problems
Whiplash Injury
The classic injury is a rear-shunt accident in a car although many other ways of getting this injury are possible.
The mechanism of injury is a complex one. As the force of the accident is applied, the thoracic spine rises up from below, compressing the neck and pushing it into an S-curve. The lower neck vertebrae, such as C5 and C6, undergo an abnormal kind of rotation, rolling backwards individually.
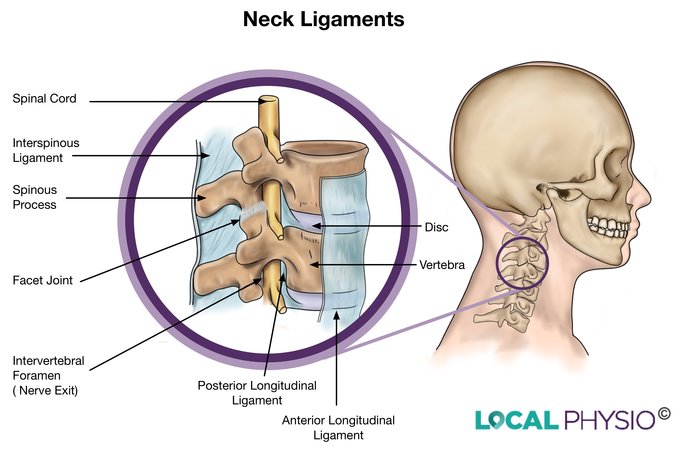
The front areas between the vertebrae are stretched and the upper half of the facet joints at the back are rammed down onto their lower halves. The lower segments extend (arch backwards) early in the movement while the upper segments are still flexing (moving forwards). These forces cause significant movement between one vertebra and another in a variety of different directions.
These movements can cause injuries to the front disc rims and fractures to the facet joints as well as tears to spinal ligaments and the facet joint capsules. Most of the anatomical structures in the neck can be injured in a whiplash even though few of these are visible on x-ray or MRI scanning.
Whiplash Severity
The severity of whiplash injury varies greatly and much debate has centred around finding a way to classify this. The main system used is the Quebec Task Force Classification as modified by Sterling (see references).
- WAD 0. No pain complaints and no findings.
- WAD 1. Neck pain, tenderness and stiffness. No signs on examination.
- WAD 2A. Neck pain. Loss of neck range of movement. Abnormal muscle activity patterns. Neck very sensitive to movement and pressure.
- WAD 2B. As 2A plus psychological distress.
- WAD 2C. As 2B plus lowered awareness of neck position, increased sensitivity to cold, heat and movement. Potential changes in sweating, reactions to cold and heat. Symptoms of acute post-traumatic stress syndrome.
- WAD3. As 2C plus neurological signs – muscle weakness, loss or alteration of feeling and loss of or decrease in reflexes.
- WAD 4. Fracture or dislocation of the neck, which is outside the diagnosis of whiplash and requires immediate emergency medical attention.
What Causes Pain In Whiplash?
The initial pain of whiplash injury is likely from the acute injuries to the neck joints, discs, nerves and ligaments. However, whiplash pain can be very severe and long-lasting and this is hard to explain just from these tissue injuries.
The nervous system can amplify its reaction to incoming sensations, giving us much higher levels of pain than normal in certain circumstances. This occurs in many chronic musculoskeletal conditions but the results in whiplash are more complex and more severe.
This condition is referred to as sensory hypersensitivity, an “over-reaction” by the nervous system to incoming stimuli. It is due to an increased excitation of the central nervous system, known as central hyper-excitability.
This makes it much easier for incoming messages about movement, pressure, vibration, cold and heat to be interpreted as pain. This process occurs very early after injury in more severe cases and can occur throughout the neck, arms and even in the lower body. This indicates a widespread disturbance of the way the central nervous system is working.
Whiplash Prognosis – How It’s Going To Go
Most people who suffer whiplash injury have:
- Mild to moderate pain
- Moderate loss of functional ability
- Increased sensitivity in the neck
- Low levels of psychological distress
- Some alteration of normal muscle function
This group of people either do well in recovering by two or three months or settle but continue with low levels of pain and loss of function.
However, around 25% to 30% of whiplash sufferers exhibit:
- More severe pain
- More severe functional loss of ability
- Widespread increased sensitivity
- Sympathetic nervous system changes – sweating, changes in blood supply and reactions to heat and cold
- Poor or abnormal function of muscle activity
- Varying degrees of post-traumatic stress
This group of people are the ones who show a poor recovery even at two years after the injury and are the most challenging to manage and treat.
Whiplash Treatment
A thorough physiotherapy assessment is vital in the acute stage of whiplash injury as this can pinpoint risk factors for a poor outcome. This allows the physio to target their treatment towards these factors, giving a greater chance of success. A conservative approach has bee shown to be more appropriate as a more aggressive approach has been shown to be associated with poorer outcomes.
It is particularly important to identify signs of post-traumatic stress disorder and high levels of pain and disability. These have been identified with the progression of acute whiplash to a long-term chronic neck pain condition.
Severe loss of movement and an exaggerated pain response to cold both predict a poor recovery and indicate that examination may aggravate symptoms unless it is performed carefully.
Physiotherapy for Whiplash
- Education about the condition
- Advice to maintain functional activities
- General exercise to maintain overall fitness
- Specific exercises to deep neck flexors and to increase neck ranges of movement
- Manual therapy
- Acupuncture
- Transcutaneous electrical nerve stimulation
- Painkillers as appropriate
- Positive coping strategies
A specific exercise and manual therapy programme has been shown to reduce pain and disability in chronic whiplash patients, but only in those without the more severe sensitivity to both movement and cold. The use of soft collars has been shown to result in poorer outcomes.
A multi-professional approach, such as a pain management programme, may be required for the group of patients with more severe symptoms.
References:
- Pernilla Åsenlöf; Annika Bring; Anne Söderlund. The Clinical Course Over the First Year of Whiplash Associated Disorders (WAD) Pain-Related Disability Predicts Outcome in a Mildly Affected Sample. BMC Musculoskelet Disord. 2013;14(361)
- Sterling M. A proposed new classification system for whiplash associated disorders – implications for assessment and management. Manual Therapy 2004; 9: 60-70.
- Jull G et al. 2008. Whiplash, Headache and Neck Pain. Research-based directions for physical therapies. Churchill Livingstone Elsevier.
Last Review Date: 11-12-2019
Next Review Date: 09-12-2021