Arthritis covers a large number of joint diseases which present with pain and stiffness in our joints. The medical specialty for these conditions is rheumatology and doctors specialising in this field are known as rheumatologists. Around 10 million people in the UK may suffer from one sort of arthritis or another. Of the many different conditions the most common are:
- Osteoarthritis (OA) – This is an age-related change in the joints characterised by bony enlargement, pain, stiffness, loss of movement and loss of function. It is both the most common type of arthritis in the world and the most disabling.
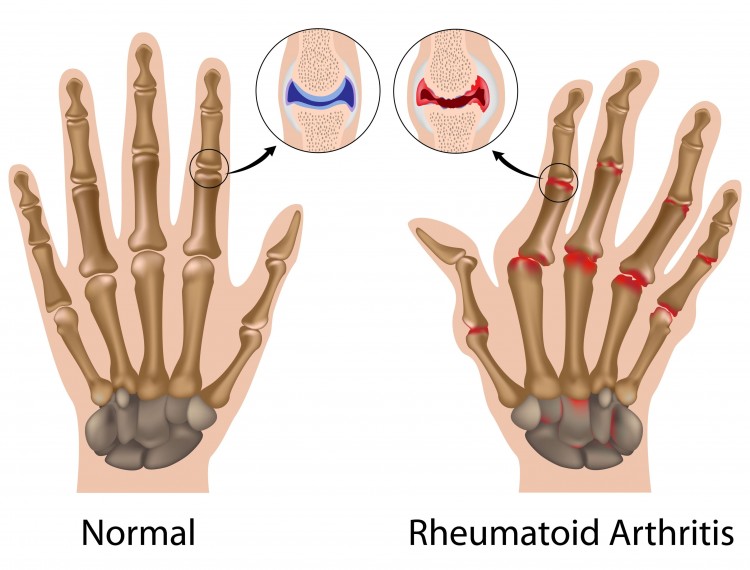
- Rheumatoid Arthritis (RA) – RA is different from OA in that it is an inflammatory arthritic disease which can lead to rapid joint damage and disability.
- Ankylosing Spondylitis (AS) – This is an inflammatory condition like RA and more common in young men. The joints stiffen and become permanently limited in movement although the pain in those areas may have passed. Usually not disabling to a great degree.
- Other inflammatory arthritic diseases such as systemic lupus erythematosus (SLE), psoriatic arthritis, childhood arthritis (juvenile rheumatoid arthritis) and gout.
What Is Arthritis?
In all forms of arthritis the main focus of damage is the articular cartilage, the smooth and friction-free covering of the joints. Cartilage allows easy movement of our joints even under load. In osteoarthritis the cartilage develops areas of localised damage and the joint responds with a repair process. If this process cannot cope with the change then the cartilage deteriorates and the nearby bone becomes denser, leading to a less functional joint. In the inflammatory disorders such as RA the immune system targets the joints, causing inflammation and local joint destruction.
Where Arthritis Occurs
The pattern of arthritis indicates to a degree what type of disease is present. OA occurs in the knees most commonly, followed by the hips, hands and spine. RA presents with widespread joint inflammation all over the body (polyarthritis) and AS tends to show itself as persistent low back pain and morning stiffness.
The Impact of Arthritis on Everyday Life
The impact of arthritis varies from the mild inconvenience of reduced hand grip or joint stiffness in the mornings to very severe disability and disturbance of daily life. The major impact comes from arthritis of the knees and hips which limits the ability to walk and get up and down from seats. Spinal arthritis may limit movement and make driving difficult from reduced neck rotation. Arthritis of the hands can interfere with opening cartons and bottles and doing up buttons and other fine tasks.
Risk Factors for Arthritis
Women have a greater chance of developing RA and men more chance of developing AS. Osteoarthritis tends to increase as a person gets older. Other risk factors may be:
- Being overweight may stress the major weight bearing joints such as knees and hips
- Someone else in the family has an arthritic condition
- Previous joint injury such as a fracture or dislocation
- Infections or surgery to a joint
- Jobs with particular stresses on joints, such as farming
Arthritis Symptoms and Signs
The initial symptoms of arthritis are commonly stiffness of a joint after use and difficulty getting going again after resting the joint. This then develops into an intermittent aching pain which can become more continuous as the problem worsens. In OA the joint under strain may click, crack or grate audibly. If a joint swells quickly or several joints are swollen then an inflammatory arthritis should be suspected. On examination doctors look for joint enlargement, swelling, loss of movement, loss of muscle power and loss of functional ability.
Do I Have Arthritis?
If you have signs and symptoms in your joint or joints then your GP is the first port of call. He or she will diagnose your problem or refer you to a specialist such as a rheumatologist if you have a less common type of arthritis. A physical examination, X-rays and blood tests are typically required to make a diagnosis and to rule out other diagnoses.
Physiotherapy and Arthritis Treatment
Physiotherapy management and self-management are vital to successful arthritis treatment as it’s a long-term condition rather than one which can be cured. Most arthritis sufferers manage their symptoms effectively and maintain their independence and quality of life.
A rheumatological physiotherapist will give an expert assessment of the state of your joints and measure pain, joint ranges, muscle power, swelling and ability to do normal tasks. They will then formulate a treatment plan which can include patient education, hydrotherapy, heat packs, mobilising and strengthening exercises, joint protection education and splints. It is important to persist with joint management over the long term as this gives the best and most predictable results. As drug treatment may have limited effectiveness and significant side effects, physiotherapy management is important for the best outcome.
Exercise for Arthritis
The National Institute for Health and Care Excellence (NICE) is the government body responsible for assessing the effectiveness of treatments for health conditions It recommends keeping physically active as a key intervention for people with arthritis. This is irrespective of the severity of pain, the age of the person, other medical problems or level of disability.
Research has shown that regular exercise is vital to keep the joints mobile, improve muscle strength and maintain aerobic fitness without increasing pain. Keeping active can also help lose excessive weight, ease the strain on affected joints, improve mobility and limit further damage.
There are three simple rules to follow:
- Choose an activity you like and can realistically do where you live
- Start slowly and build up gradually
- Do it regularly
A physiotherapist can develop a plan of suitable activities, and advise you on safety precautions as well as special equipment you may have to use. In studies, exercising regularly under the guidance of a physiotherapist has been associated with reductions in pain and better functioning. In people with osteoarthritis after total knee replacement, improved recovery has been demonstrated. Physiotherapists can also provide manipulation and stretching for an arthritic joint, especially an osteoarthritic hip.
Tips for Managing Arthritis
Physiotherapists can suggest many simple, effective ways of managing your arthritic joints and these ideas can include:
- Maintaining good posture overall
- Maintaining the ranges of your joints to prevent deformities developing
- Integrating an exercise programme into your daily regime
- Pacing your daily activities to prevent overexerting yourself and suffering after
- Joint protection strategies such as opening a door with an arm rather than the wrist and hand or sliding objects on a surface rather than lifting them.
- Using tools for the kitchen and garden that are adapted or are lighter with larger handles
References:
- Arthritis Care, About Arthritis, 2014;
- Arthritis Research UK and The Chartered Society of Physiotherapy, Physiotherapy and Arthritis, April 2011;
- Arthritis Research UK, How Can Physiotherapy help?
- Lowe Minns CJ, Barker KL, Dewey M, Sackley CM. Effectiveness of physiotherapy exercise after knee arthroplasty for osteoarthritis: systematic review and meta-analysis of randomised controlled trials. British Medical Journal, October 18, 2007; doi:
- NHS Choices, Arthritis – Introduction, February 21, 2014;
- National Institute for Health and Care Excellence (NICE). Osteoarthritis – Care and Management in Adults, February 2014;
Last Review Date: 24-02-2017
Next Review Date: 23-06-2019